The AI Intelligence Layer for Pre-Bill Revenue Integrity
Purpose-built AI applications that detect and resolve revenue risk before claims are submitted.
Built for healthcare finance teams · Specialty-aware · No rip-and-replace
"Revenue doesn't break at submission. It breaks before it."
Most organizations focus on denials after claims are rejected. But revenue loss starts earlier — in documentation gaps, eligibility errors, missing authorizations, and coding inconsistencies.
Purpose-built AI applications. Powered by Grelin
Each application targets a specific pre-bill revenue risk — all powered by the same intelligence engine.
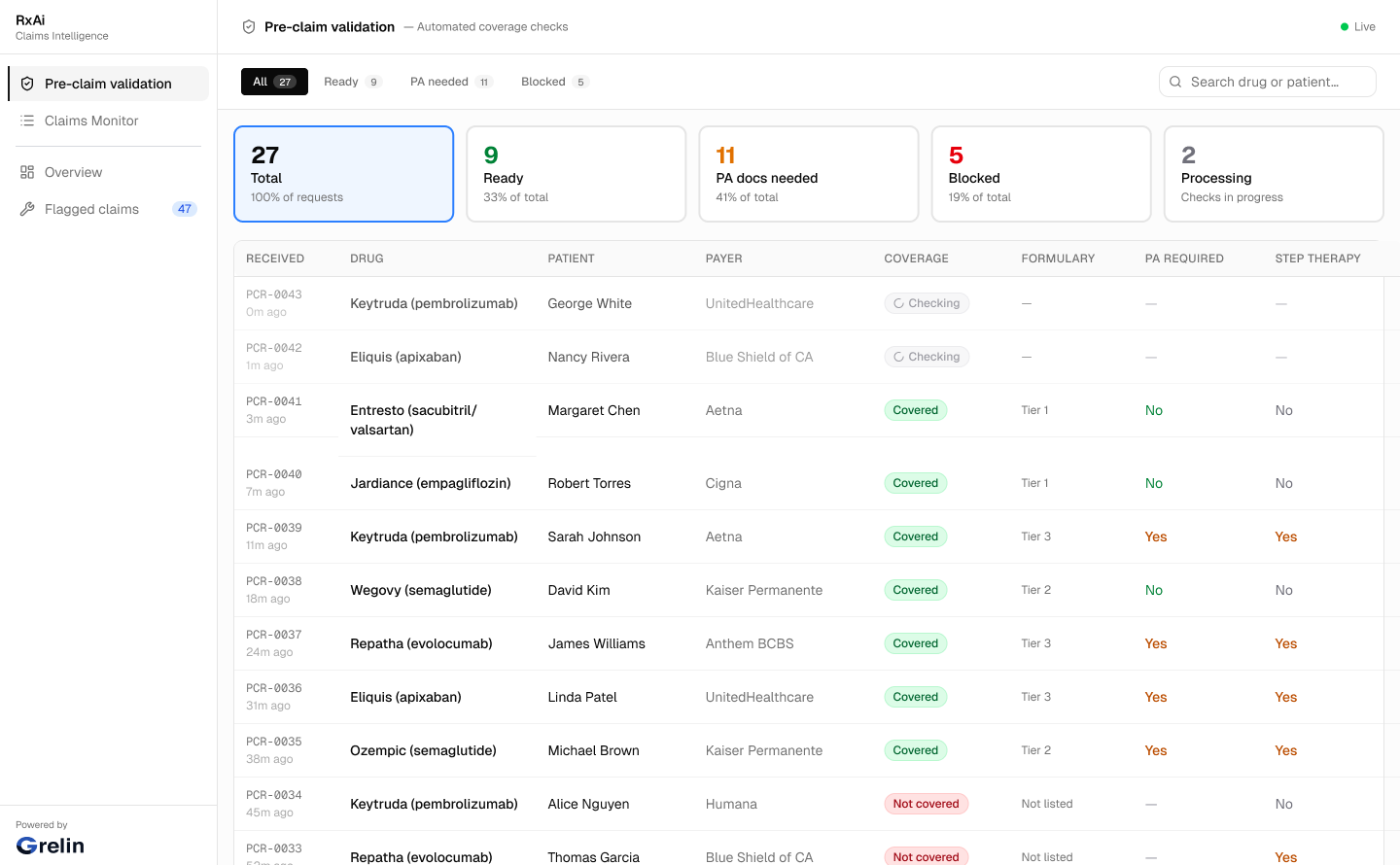
Rx.ai
Prescription claim integrity before dispensing. Catch documentation and coverage gaps before they become denials.
Explore Rx.ai →Wound.ai — Audit Review
Patient #3847 · Sarah M. · Admitted 04/01/26
| Wound type | Pressure ulcer — sacral | Gap |
| ICD-10 code | L89.313 · L89.154 | Verified |
| Debridement | Note missing 04/03 | Review |
| Photo doc. | 2 of 4 uploaded | Incomplete |
| Complexity | Multi-wound · 3 sites | Flag |
| Measurements | Dimensions not recorded | Missing |
4 documentation gaps detected
Est. $2,640 at risk · Pre-bill action required
Wound.ai
Pre-bill revenue intelligence for wound care complexity. Reduce documentation gaps and denial exposure.
Explore Wound.ai →Pain.ai — Code Validation
Epidural steroid inj. · CPT 64483 · 04/09/26
Validation Score
3 of 5 checks passed
Action required before submission
Risk: Medium · 2 code issues flagged
Modifier 59 conflict · Diagnosis linkage incomplete
Pain.ai
AI-powered billing validation for pain management. Prevent coding and documentation misalignment before submission.
Explore Pain.ai →PriorAuth.ai — Gap Scan
Claim #PA-2024-881 · Multi-procedure · 04/09/26
Spine injection L3–L4
Auth #AUT-4412 · valid thru 06/30/26
MRI lumbar w/ contrast
No active authorization on file
PT sessions — 12 req.
6 of 12 approved · renewal pending
Lab panel — CBC/CMP
Payer response awaited · sent 04/07
Fluoroscopy guidance
Bundled with spine auth · confirmed
2 upstream gaps · Est. $3,200 at risk
MRI auth missing · PT partial approval
PriorAuth.ai
Detect authorization gaps before they delay reimbursement. Reduce friction and prevent claim disruption.
Explore PriorAuth.ai →John Doe · DOB 04/15/1972
BlueCross PPO · Member XY-8821043
⚠ Coverage lapsed — verify eligibility before service
Last active: 12/31/25 · Renewal not confirmed
| Effective date | 01/01/26 – 12/31/25 | Lapsed |
| Network status | In-network (PPO) | Verified |
| Deductible | $1,200 remaining | Alert |
| Copay | $40 specialist visit | OK |
| Out-of-pocket | $3,500 max · $2,100 met | Tracking |
| Authorization | Required for this svc | Missing |
Eligibility.ai
Catch coverage and eligibility breakdowns upstream. Minimize preventable claim rejections tied to payer verification.
Explore Eligibility.ai →Prescription claim integrity before dispensing. Catch documentation and coverage gaps before they become denials.
Explore Rx.ai →
Grelin is not a single RCM tool
AI Intelligence Layer
An AI Intelligence Layer embedded into your existing healthcare workflows — analyzing clinical and financial signals before submission to detect risk, prevent breakdowns, and optimize performance.
Purpose-Built Apps
Each Grelin application solves a specific pre-bill challenge. Every application is powered by the same intelligence engine.
Built to Scale
As your organization grows, the intelligence grows with it.

Built for high-scrutiny specialities
Our platform is engineered for the complex clinical documentation and rigorous audit environments of specialized care.
Wound Care
Intelligent documentation analysis for complex clinical cases, ensuring every stage of healing is accurately captured and billed.
Pain Management
Automated pre-bill verification for interventional procedures, managing rigorous authorization requirements without slowing throughput.
MSO & Multi-Specialty
Centralized revenue intelligence for multi-facility operations, providing uniform quality standards across a diverse portfolio.
What happens when revenue intelligence moves upstream
Catch issues before they become denials. Grelin surfaces pre-bill risk across documentation, eligibility, authorization, and coding.

Revenue Health Overview
Preventable Denials
Caught upstream before submission
Our AI-driven engine identifies gaps in authorization and coding documentation in real-time, preventing high-risk claims from moving downstream.
Performance Metrics
Automated risk detection at scale
Consistent pre-bill validation
Fewer surprises, fewer rework cycles
Let's Connect!
Precision Intelligence.
See where your revenue is at risk
before claims go out the door
Grelin identifies pre-bill revenue risk across documentation, eligibility, authorization, and coding before it becomes a denial.



